Five Year Population Health Strategy
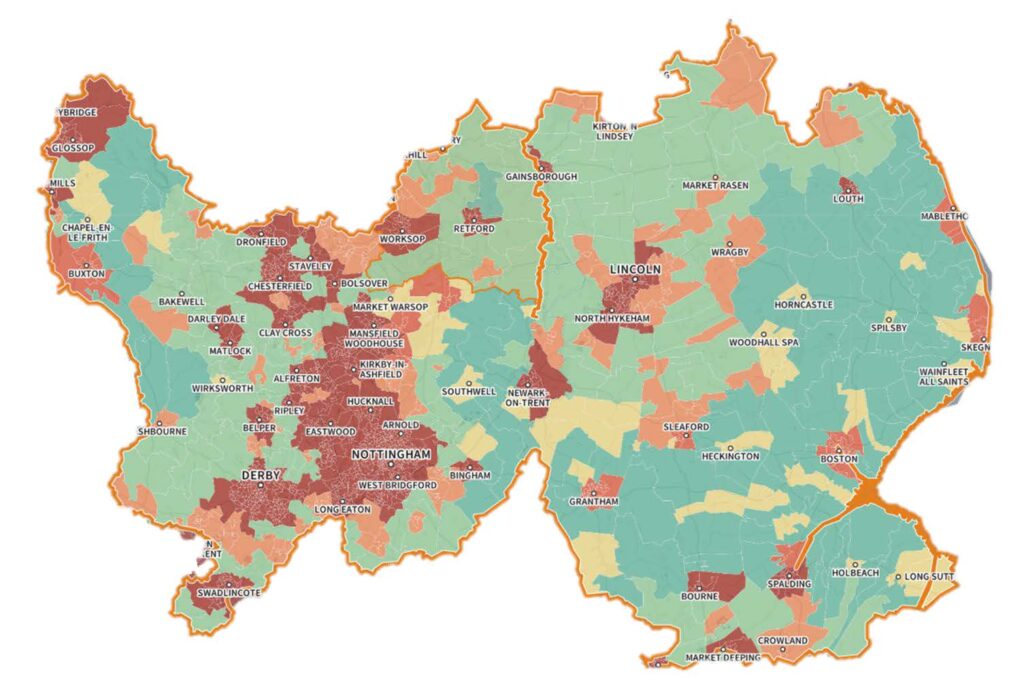
The Five Year Population Health Strategy for the Derby and Derbyshire, Lincolnshire, Nottingham and Nottinghamshire (DLN) Cluster explains how we plan to help people live longer, healthier lives.
It sets out how the NHS, working alongside Local Authorities and voluntary and community partners, will improve people’s access to care and reduce the unfair differences in health that exist across our communities.
Our vision
Every person in every community will live longer and healthier lives. We will improve population health outcomes, reduce inequalities and ensure equitable access across Derby & Derbyshire, Lincolnshire and Nottingham and Nottinghamshire.
What our citizens are telling us and our priorities
Neighbourhood Health: The Engine Room
We will deliver our priorities through neighbourhood health, making sure that GP practices, community teams, mental health services and others are joined up and working as one team for their neighbourhood. We will also focus on things that make the biggest difference to long‑term health, like healthy lifestyles, good early years development, strong social connections, and support for people who are most excluded or at risk.
Expected system-wide impact
Successful delivery of our Population Health Strategy will support:
- More people to live longer in good health
- Fewer preventable crises
- Reduced inequalities in access, experience and outcomes
- A significant hospital to community ‘shift’
- Better use of NHS resources and improved financial sustainability.
Home – NHS Nottingham and Nottinghamshire ICB | Joined Up Care Derbyshire Integrated Care System.